Introduction
Pain, in many forms, is part of the human experience. Whether from sports injuries, chronic conditions, or everyday stress, people of all ages in Stamford CT seek relief that is safe and sustainable. Historically, pain treatment often relied heavily on medications without exploring the wider picture of lifestyle, prevention, or emotional wellbeing. In recent years, healthcare professionals have shifted toward more comprehensive approaches that include physical, emotional, and environmental factors.
At the same time, pain management continues to inspire important conversations. How do providers balance effective relief with safety. How do we encourage healthy recovery while being cautious about medications that require supervision and regulation. As research grows and public awareness increases, primary care practices in Stamford are rethinking how to support patients with science based strategies. This topic affects teens, adults, and older residents alike, making it both significant and relevant in today’s healthcare landscape.
Unpacking the layers of pain management options in Stamford CT
Primary care providers focus on understanding the cause of pain before choosing treatment. A visit usually starts with questions about when the pain began, how it feels, and what makes it better or worse. Providers may review medical history, past injuries, daily routines, sleep patterns, and stress levels. This helps identify whether pain is related to muscle strain, chronic illness, inflammation, or lifestyle habits. The Centers for Disease Control and Prevention offers educational information on safe pain care and chronic pain topics (https://www.cdc.gov).
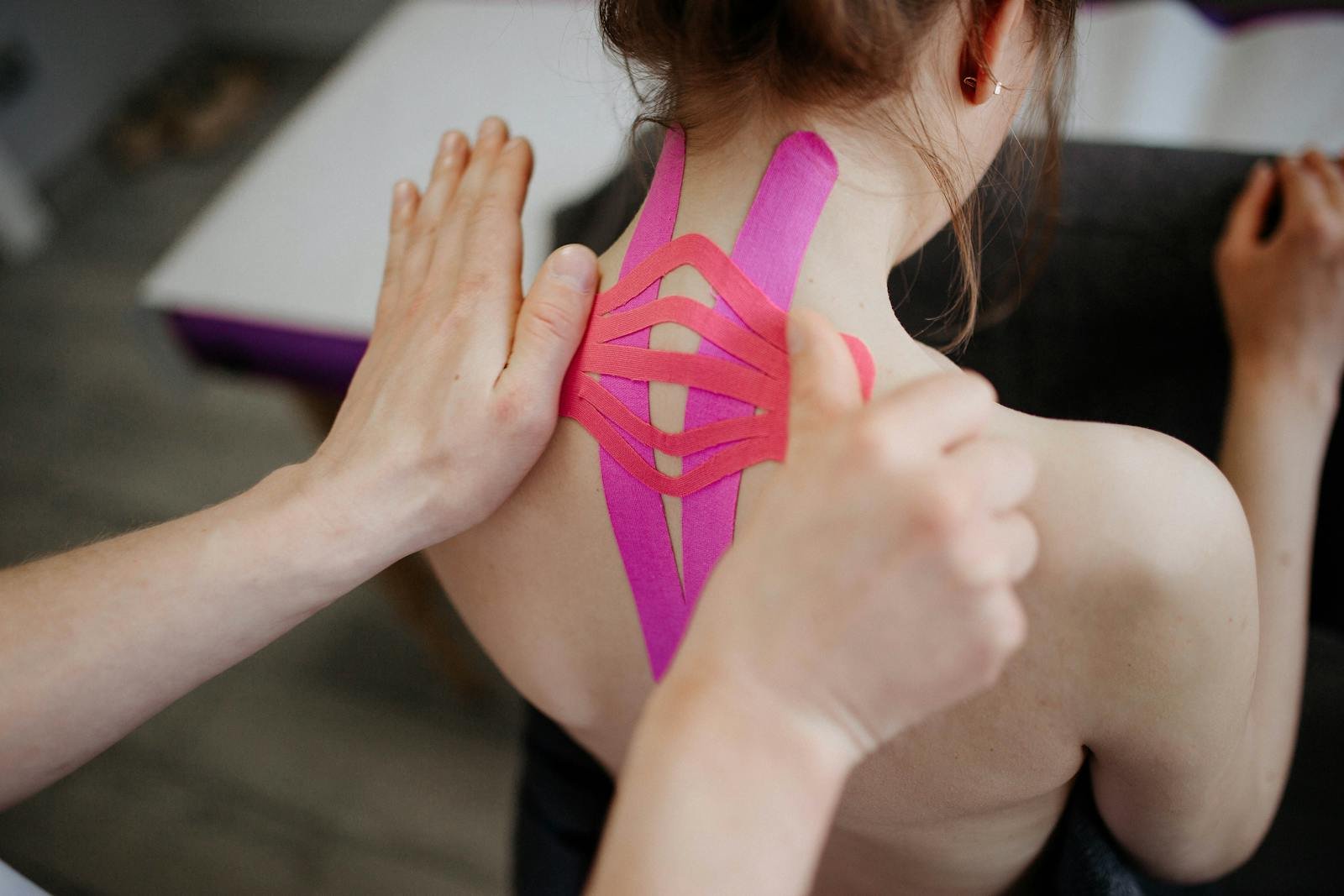
Many primary care practices encourage non medication strategies first when appropriate. Stretching routines, gentle movement, and physical therapy referrals support mobility and reduce discomfort over time. Ice, heat, and ergonomic changes, such as adjusting posture or screen habits at home or school, can also be important.
Some patients benefit from short term medications prescribed and monitored by licensed professionals. These decisions involve careful evaluation of risks and benefits. Mental wellbeing plays a major role in pain perception, so providers often discuss stress reduction, mindfulness, or counseling options. The National Institutes of Health provides useful background information about pain science and treatments (https://www.nih.gov).
Navigating the challenges and debates
Pain management includes complex debates about medication safety, access, and potential risks. In recent years, national conversations highlighted concerns about certain prescription pain medicines. Primary care providers follow strict safety guidelines and do not recommend controlled substances without clear medical necessity and supervision. In many cases, providers consider alternatives such as physical therapy, behavioral support, or specific exercises.
Another ongoing discussion involves how pain can affect emotional wellbeing. People sometimes feel discouraged when pain limits activities or social connections. Healthcare professionals encourage open communication and supportive conversations rather than ignoring discomfort. Research from the Agency for Healthcare Research and Quality explores chronic pain, safe treatment approaches, and decision making in healthcare (https://www.ahrq.gov).
There are also questions about how digital information influences pain management. Some online suggestions promote unproven supplements or extreme methods that may not be safe. Primary care practices emphasize evidence based strategies and encourage patients to discuss options before trying something new.
Equity is another concern. Access to physical therapy, specialist appointments, or preventive programs may vary across communities. Stamford primary care practices continue to explore ways to make supportive care more accessible, including telehealth check ins that help families stay connected to care.
Real world echoes: case studies and applications
Imagine a Stamford teen who develops knee discomfort after joining a new sport. Instead of relying only on over the counter remedies, they visit a primary care provider. After reviewing activity levels and performing a physical exam, the provider recommends stretching routines, rest from intense activity for a short period, and a gradual return with proper warm ups. The teen also learns injury prevention techniques for future sports seasons.
Another fictional example involves an adult who experiences frequent back pain from long workdays. Their primary care provider asks about posture, workstation setup, and daily stress. With guidance, the patient adjusts chair height, takes stretch breaks, and practices gentle core strengthening exercises. Over several weeks, symptoms improve without requiring heavy medication.
Telehealth plays a growing role in pain management. Secure video visits allow patients to review symptoms and discuss strategies without missing school or work. Providers may suggest home exercises or refer individuals to physical therapy. Mental wellness conversations, including stress management, can also take place during virtual visits. These examples show how pain management goes beyond medication and becomes a collaborative process.
Conclusion
Pain management offered by Stamford primary care providers reflects a thoughtful shift toward whole person care. Instead of relying only on medications, modern approaches blend lifestyle strategies, education, and supportive communication. While debates continue about access, equity, and responsible prescribing, primary care teams focus on helping patients understand pain, stay active safely, and explore personalized strategies. Readers are encouraged to seek trustworthy information, ask questions during appointments, and remember that effective pain care is a journey rather than a quick fix. To learn about local services or schedule a consultation, consider contacting CNPprimarycare.com.
Q and A
What happens at a pain management appointment
Primary care providers ask about symptoms, lifestyle, past injuries, and daily routines. They work with patients to build safe strategies based on individual needs. The CDC provides general education on chronic pain topics (https://www.cdc.gov).
Do all pain treatments involve medication
Not necessarily. Many people benefit from physical therapy, stretching, posture changes, and stress management strategies. Only licensed professionals determine whether medication is appropriate.
What if pain affects school or work
Talk openly with a healthcare provider. They can suggest practical adjustments, supportive exercises, and strategies that fit your daily routine. The National Institutes of Health offers information on pain and healthy living (https://www.nih.gov).
How can Stamford residents learn more
Primary care practices, community programs, and telehealth services provide pain management guidance. If you want local support or personalized care, you can contact CNPprimarycare.com for services and information.